Undergoing a tooth removal is a common dental procedure, yet the recovery period often brings about various questions regarding what is part of the natural healing process and what is a cause for concern. Many patients ask: is an infection after tooth extraction normal? While the body’s inflammatory response naturally causes some soreness, a true bacterial infection is a post-operative complication that requires prompt attention.
Modern oral surgery utilizes high sterilization standards to minimize risks, but the mouth is naturally home to billions of bacteria. When a tooth is removed, it leaves an open "socket" in the bone. If bacteria infiltrate this area or if the body's immune response is compromised, a gum infection after extraction tooth may develop. Distinguishing between the typical "healing blues" and a clinical infection is the first step toward a safe recovery.
Table of Content
Common Signs of Infection After Tooth Extraction
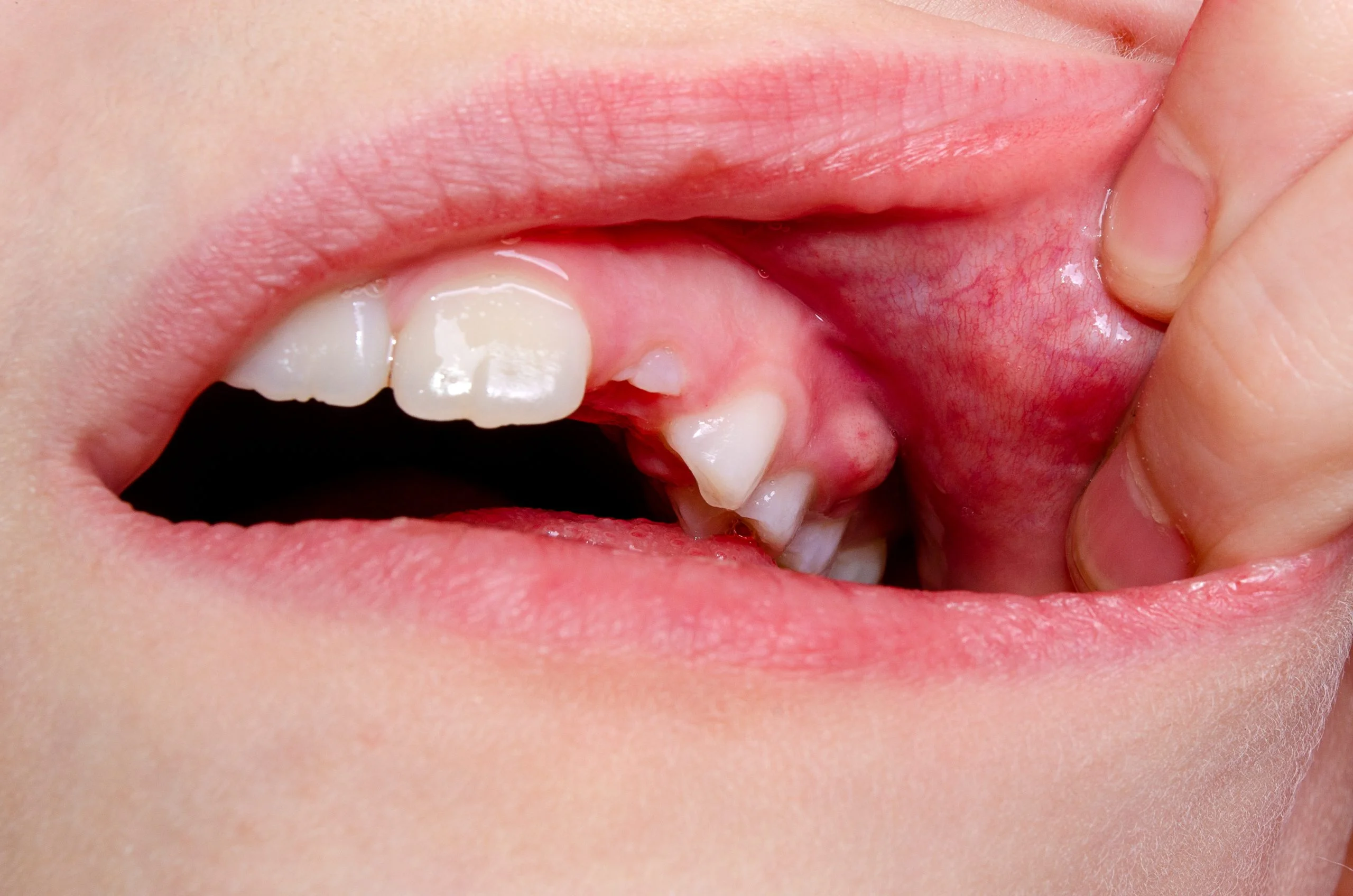
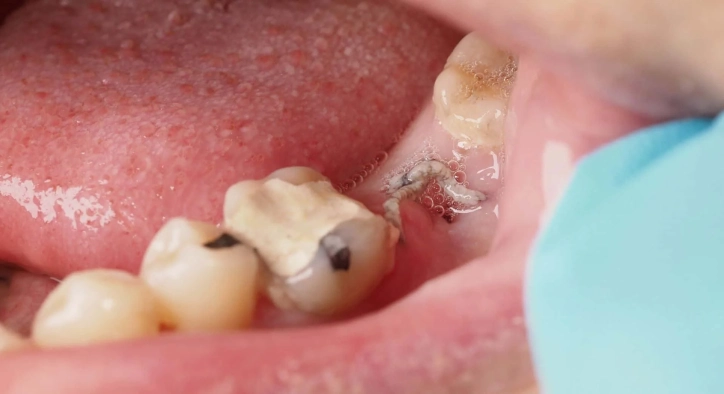
Knowing how to tell if tooth extraction is infected or just healing can be difficult in the first 48 hours. Generally, normal healing pain peaks around the second day and then gradually subsides. However, if your pain intensifies after day three, you might be dealing with an infected socket after tooth extraction.
The most frequent signs of infection after tooth extraction include:
- Persistent Swelling: While some facial swelling is expected, it should begin to diminish after 72 hours. If the swelling increases or feels warm to the touch, it may indicate a gum infection after tooth extraction.
- Foul Odor or Taste: A persistent bitter taste or an unpleasant breath odor that does not go away with gentle rinsing is often caused by the presence of bacteria and pus.
- Discharge: Seeing white or yellow fluid oozing from the site is one of the clearest signs of gum infection after tooth extraction.
- Fever and Chills: If your body temperature rises above 38°C (100.4°F), it suggests the infection might be spreading systemically.
- Limited Jaw Opening: While some stiffness is normal, an inability to open the mouth (trismus) that worsens over time is a red flag.
In rare and more severe cases, patients might experience bone infection after tooth extraction symptoms, such as deep, radiating jaw pain, or even numbness in the lip and chin area. These symptoms suggest the bacteria have moved beyond the soft tissue into the underlying mandibular or maxillary bone.
Why Does Infection After Tooth Extraction Occur?
An infection after tooth extraction rarely happens without a contributing factor. The oral cavity is a complex environment, and several elements can disrupt the delicate balance of the healing socket.
- Pre-existing Infection: If the tooth was removed due to a severe abscess, bacteria might already be present in the surrounding tissues.
- Poor Oral Hygiene: Failing to follow tooth extraction aftercare instructions can lead to food debris and plaque accumulating in the open wound.
- Smoking and Vaping: Tobacco use reduces blood flow to the gums and introduces contaminants, significantly slowing down the healing process and increasing the risk of a gum infection after extraction tooth.
- Medical Conditions: Patients with weakened immune systems, such as those with uncontrolled diabetes or those undergoing chemotherapy, may face a higher risk.
- Complexity of Surgery: Impacted wisdom teeth often require more invasive techniques, which naturally creates a larger area for potential bacterial colonization.
Dry Socket or Infection? How to Spot the Difference
Many patients confuse a "dry socket" (alveolar osteitis) with an infection after tooth extraction. While both are painful, they are biologically different. A dry socket occurs when the blood clot that is supposed to protect the bone dissolves or dislodges prematurely, exposing the bone and nerves to air and food.
What does an infected tooth socket look like? An infected socket usually appears red, swollen, and may have visible pus. In contrast, a dry socket often looks "empty." You might see the white or grayish color of the underlying bone instead of a dark blood clot. While dry socket pain is intense and radiating, it is not always accompanied by the fever or pus found in a bacterial gum infection after tooth extraction.
Professional Treatment for Infection After Tooth Extraction
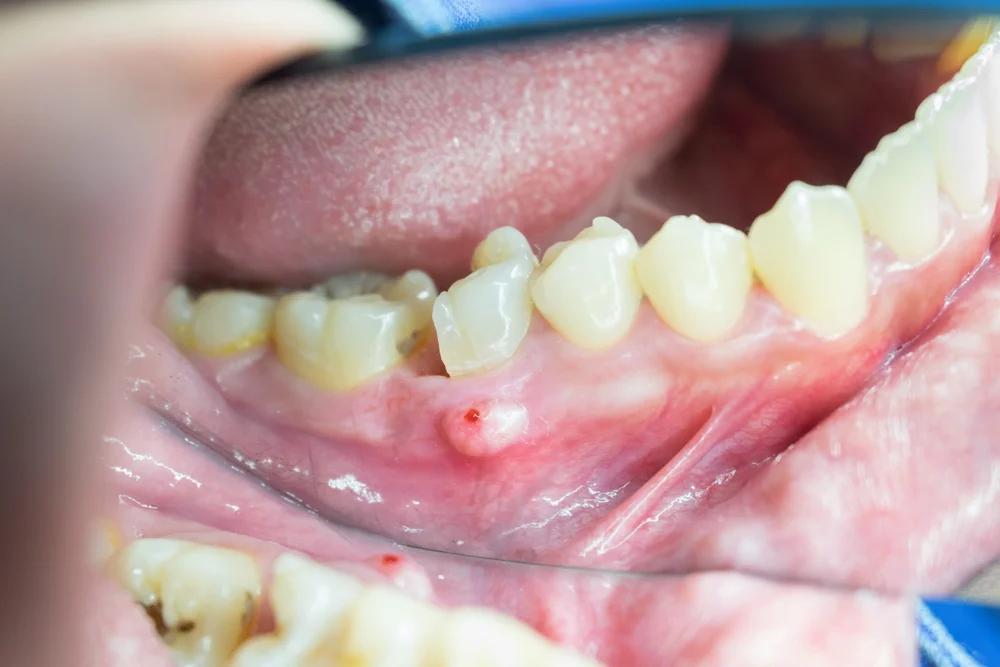
If you suspect you have an infected socket after tooth extraction, you might wonder, "can a tooth extraction infection go away on its own?" Unfortunately, dental infections are trapped within the tissue or bone and rarely resolve without intervention. Waiting too long can allow the bacteria to spread to other parts of the head and neck.
When you ask your dentist how to treat infection after tooth extraction, the clinical approach usually involves:
- Debridement and Irrigation: The dentist will gently clean the socket to remove food particles and infected tissue. They often flush the area with a sterile saline solution or an antibacterial rinse.
- Antibiotics after extraction: If the infection is spreading or if the patient is at high risk, a course of antibiotics after extraction is typically prescribed. It is essential to finish the entire course even if symptoms improve quickly.
- Medicated Dressings: In cases involving dry socket or localized infection, a medicated paste may be placed in the socket to soothe pain and provide an antimicrobial barrier.
- Drainage: If a dental abscess has formed in the gums, the surgeon may need to make a small incision to drain the accumulated fluid.
How to Prevent Post-Surgical Complications at Home
The best way to handle an infection after tooth extraction is to prevent it from starting. Successful tooth extraction aftercare is a partnership between the surgeon’s skill and the patient’s diligence at home.
- The 24-Hour Rule: During the first day, do not rinse your mouth vigorously, spit, or use a straw. These actions can dislodge the blood clot, leading to a dry socket or an infected socket after tooth extraction.
- Saltwater Rinses: After the first 24 hours, gently bathe the area with warm salt water (1/2 teaspoon of salt in a cup of water) several times a day. This helps keep the area clean and reduces the bacterial load.
- Dietary Choices: Stick to soft foods like yogurt, mashed potatoes, or soup (not hot). Avoid crunchy or seedy foods that could get lodged in the healing site.
- Keep it Clean: Continue to brush your other teeth, but be extremely careful around the extraction site.
- Rest: Avoid strenuous physical activity for at least 48 hours, as increased heart rate can lead to post-operative bleeding and swelling.
FAQ
Can I treat an infected tooth extraction at home?
While salt water rinses can help keep a healthy mouth clean, they cannot cure a deep-seated infection after tooth extraction. If you see pus or have a fever, home remedies are insufficient. You need a professional evaluation to determine if antibiotics after extraction or clinical cleaning is required.
Is yellow discharge normal after tooth extraction?
It depends on the appearance. A thin, yellowish-white film (called slough) that stays attached to the socket is often a normal part of the healing tissue. However, if the yellow discharge is thick, creamy, or can be wiped away and is accompanied by a foul smell, it is likely pus, indicating a gum infection after tooth extraction.
How long after an extraction can an infection start?
Most infections manifest between 2 to 7 days after the procedure. If you have been feeling better and suddenly experience a resurgence of pain and swelling on day 4 or 5, an infected socket after tooth extraction may be the cause.
Will I need more surgery if my socket is infected?
In most cases, no. A thorough cleaning and a course of antibiotics are usually enough. However, if a severe bone infection after tooth extraction symptoms are present, a minor follow-up procedure to remove damaged bone tissue might be necessary.
Is bad breath normal after tooth extraction?
A slight change in breath is common due to the blood clot and the inability to brush the area thoroughly. However, a "rotting" smell or a constant foul taste is one of the classic signs of dental infection and should be checked by your dentist.
When to call a dentist for post-extraction pain?
You should call your dentist if your pain is not controlled by prescribed medication, if swelling increases after the third day, or if you develop a fever. Early intervention makes how to treat infection after tooth extraction much simpler and faster.