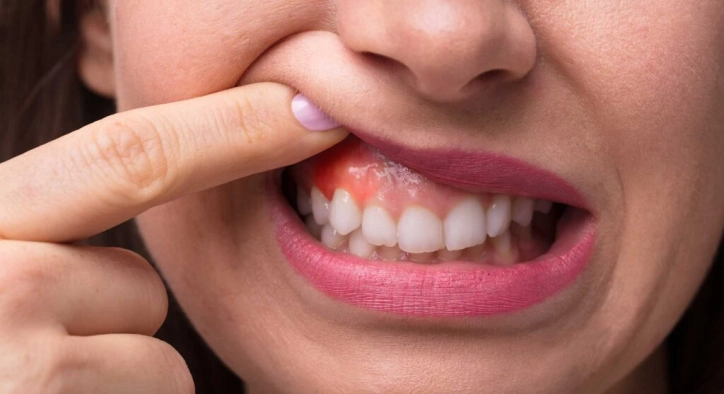
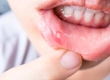
Gum Pain has a sneaky way of turning ordinary moments into tiny dramas: a sip of cold water suddenly feels like a plot twist, floss becomes a suspense scene, and smiling for a photo requires strategy. At Stamboul Clinic, we often meet people who assumed their discomfort was “nothing,” only to realize the gums are excellent messengers. They rarely shout without a reason.
İçindekiler
- The Science of Gum Pain: What Your Gums Are Trying to Tell You
- Everyday Triggers of Gum Pain (And Why They Happen)
- When Gum Pain Points to Gum Disease: Gingivitis vs Periodontitis
- Localized Gum Pain Around One Tooth: Abscess, Food Traps, and Dental Work
- Fast Comfort Strategies for Gum Pain: What People Commonly Try
- Gum Pain and Hormones, Medications, and Dry Mouth: The Underestimated Trio
- When Gum Pain Becomes a Red Flag: Timing, Swelling, and Systemic Clues
- How Dentists Investigate Gum Pain: The Tools Behind the Answer
- Turning Gum Pain Into Useful Information
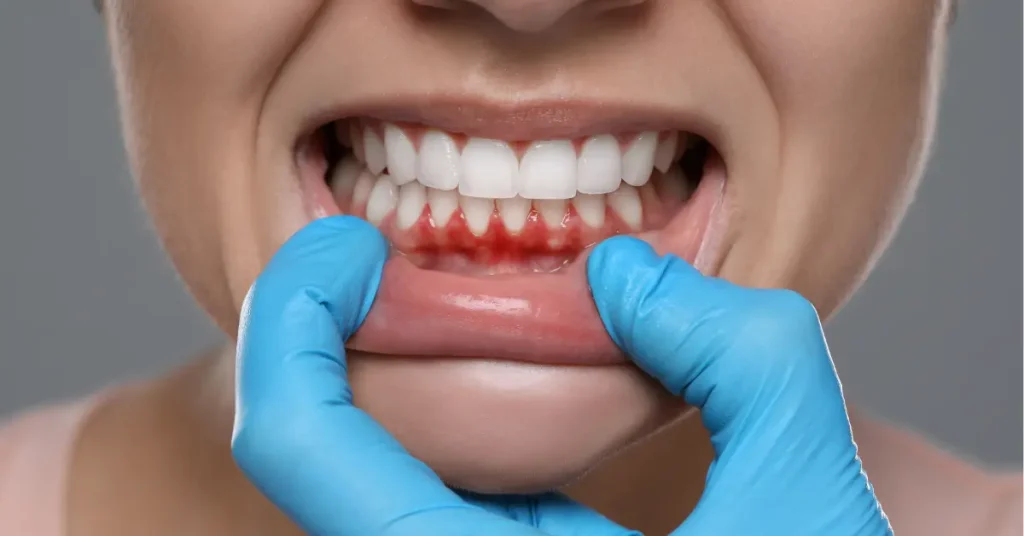
The Science of Gum Pain: What Your Gums Are Trying to Tell You
Gum Pain isn’t a diagnosis; it’s a signal. Gum tissue contains nerve endings, blood vessels, and immune cells that respond quickly to irritation. When something disrupts the balance of the mouth (plaque, friction, chemicals, or infection), inflammatory messengers such as cytokines can increase local sensitivity. That’s when the gums may feel sore, tender, swollen, or “raw.”
People describe Gum Pain in different ways, and those differences can be meaningful. A dull ache around one tooth can feel different from a burning sensation along the gumline, and both can differ from throbbing pain that wakes you up. The mouth is small, but it hosts a complex ecosystem, and pain is often the first clue that the ecosystem is under pressure.
Another important point: gum tissue is designed to be resilient, yet it heals best in a clean, low-irritation environment. If irritation continues (for example, plaque staying in place near the gumline), the body’s immune response can keep running like an engine stuck at high RPM. That “high RPM” feeling may show up as Gum Pain, bleeding, tenderness, or a change in gum color.
Everyday Triggers of Gum Pain (And Why They Happen)
Many cases of Gum Pain begin with simple, everyday triggers rather than dramatic emergencies. One common driver is plaque buildup. Plaque is a sticky biofilm that forms naturally; if it isn’t disrupted consistently, it can irritate the gum margin. This may lead to gingival inflammation that feels sore when brushing, flossing, or chewing.
Mechanical irritation is another frequent cause. Brushing with a hard-bristle brush, applying too much pressure, or using a sawing motion can scrape the gumline over time. Floss can also irritate if it “snaps” into the gums. Even small habits, repeated daily, can create a big sensory outcome: persistent Gum Pain.
Lifestyle factors can add their own layer. Smoking and vaping are often associated with changes in gum tissue response and healing capacity. Stress may contribute indirectly by affecting immune regulation and encouraging clenching or grinding, which can make the tissues feel tender. None of these factors guarantees discomfort, but they can raise the odds that Gum Pain appears and lingers.
When Gum Pain Points to Gum Disease: Gingivitis vs Periodontitis
Sometimes Gum Pain is the early “check engine” light of gum disease. Gingivitis is typically discussed as inflammation of the gums that can involve redness, swelling, tenderness, and bleeding with brushing. It is often linked with plaque accumulation at the gumline. At this stage, the irritation is mainly in the soft tissue, and many people notice changes in comfort before they notice visible changes.
Periodontitis is generally described as a more advanced process that can affect the supporting structures around teeth. This may involve deeper gum pockets, gum recession, and changes in bone support. Not everyone feels intense pain with periodontitis; paradoxically, some people report minimal discomfort while damage progresses quietly. Still, Gum Pain can occur, especially during flare-ups or when an area becomes acutely inflamed.
To make the difference easier to visualize, here is a simplified comparison people often find useful:
Feature | Gingivitis (often earlier stage) | Periodontitis (often more advanced) |
Common sensations | Tenderness, mild Gum Pain, bleeding | Tenderness, episodic Gum Pain, possible chewing discomfort |
Typical visible signs | Redness, swelling | Recession, pocketing, tooth mobility in some cases |
What’s happening | Inflammation mainly in gums | Inflammation plus support tissue involvement |
This table is a learning tool, not a diagnostic checklist. Still, it shows why persistent Gum Pain deserves attention rather than “waiting it out.”
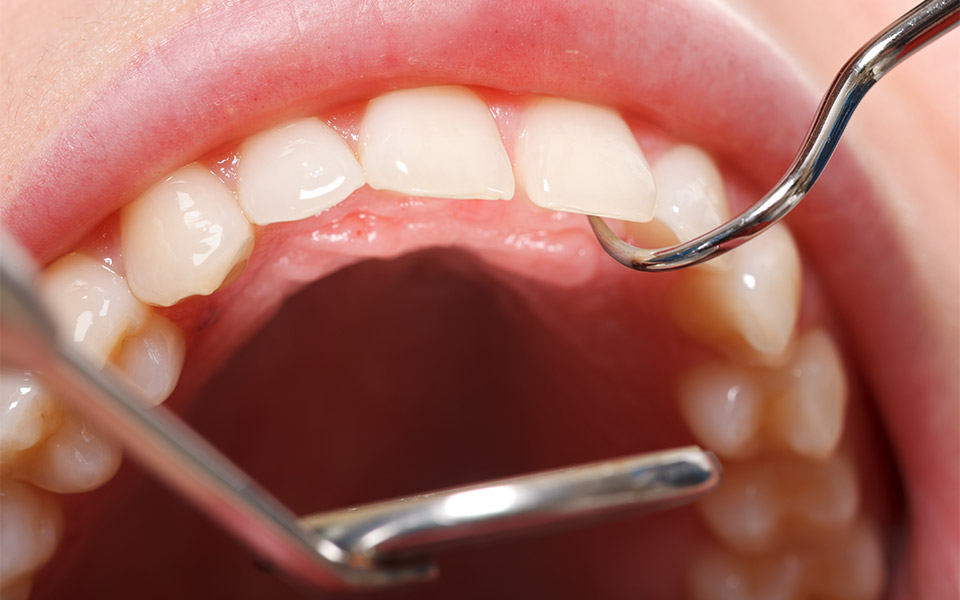
Localized Gum Pain Around One Tooth: Abscess, Food Traps, and Dental Work
When Gum Pain is sharp and localized to one spot, people often suspect “something stuck,” and they are sometimes right. Food traps between teeth can press into the gum papilla and create soreness, especially after eating fibrous foods. That localized irritation may feel like a tiny bruise in the gum.
In other cases, localized Gum Pain can be associated with an abscess or infection. People may describe a pimple-like bump, pressure, bad taste, or swelling. These scenarios tend to feel different from generalized sensitivity because the discomfort can become more intense and focused. Because infections can behave unpredictably, a dental evaluation is usually the most informative next step.
Dental procedures can also temporarily change how gums feel. A recent cleaning, new crown margin, orthodontic movement, or ill-fitting restoration can irritate the gumline. Even a well-done procedure may leave tissues slightly inflamed while they adapt. If Gum Pain appears after dental work, timing and location are useful clues when discussing the issue with a clinician.
Fast Comfort Strategies for Gum Pain: What People Commonly Try
When Gum Pain shows up, most people want two things: comfort now and a plan for later. While you should avoid self-diagnosing, it can help to understand the categories of relief approaches commonly mentioned in dental settings.
First, many people focus on reducing irritation. That might mean switching to a softer toothbrush, slowing down the brushing motion, and cleaning gently along the gumline. If flossing triggers Gum Pain, technique adjustments can make a difference: guiding the floss in a controlled way rather than snapping it down can reduce trauma.
Second, people often use rinsing habits for temporary soothing. Mild saltwater rinses are frequently discussed as a simple comfort measure, largely because they can feel calming and help flush debris. Some over-the-counter mouth rinses are marketed for gum care; however, formulas vary widely, and some can be harsh if used incorrectly or too often. If a rinse causes burning or worsens Gum Pain, that reaction is worth noting.
Third, consider what you chew. Hard, crunchy foods can aggravate tender tissues. Softer foods and avoiding extremes of heat and cold can make Gum Pain easier to live with while you observe what’s going on. Comfort matters, but it shouldn’t replace figuring out the cause.
If you want a quick, practical checklist of low-friction habits people commonly choose during a sore-gum period:
- Use a soft-bristle brush and gentle pressure
- Clean interdentally carefully (floss or interdental brushes as appropriate)
- Rinse gently after meals to reduce debris
- Avoid smoking or vaping while tissues are irritated
- Note patterns: when Gum Pain spikes, where it’s located, and what triggers it
Gum Pain and Hormones, Medications, and Dry Mouth: The Underestimated Trio
Not all Gum Pain starts with brushing. Hormonal changes can influence gum tissue response, blood flow, and inflammation sensitivity. Some people notice gum tenderness during periods of hormonal fluctuation. The gums may appear more reactive to plaque even when oral hygiene habits haven’t changed dramatically.
Medications can also play a role. Certain drugs are associated with dry mouth (reduced saliva), and saliva is a major protective factor. It buffers acids, supports mineral balance, and helps control microbial growth. When saliva is low, the mouth can feel sticky, tissues can become more fragile, and Gum Pain can become easier to trigger.
Dry mouth can also be influenced by hydration, mouth breathing, and some systemic conditions. If you wake up with a dry mouth and Gum Pain near the front gums, for instance, nighttime mouth breathing can be one of several plausible contributors. The key idea is that comfort is not only about teeth and plaque; it’s also about the mouth’s moisture, chemistry, and friction levels.
For additional background on gum health basics, you can review educational material from the American Dental Association and public health guidance from the CDC. These resources help frame how clinicians think about gums in a broader health context.
When Gum Pain Becomes a Red Flag: Timing, Swelling, and Systemic Clues
Most people want a simple rule: “When is Gum Pain serious?” Dentistry rarely gives perfect yes-no rules, but patterns matter. Pain that persists, escalates, or repeatedly returns to the same location often deserves closer attention. Swelling that changes the shape of the gumline, drainage, a bad taste, or pain that interferes with sleep can be meaningful clues.
Another important context is systemic symptoms. If gum discomfort appears alongside feverish feelings, facial swelling, or difficulty opening the mouth, it may signal a situation that shouldn’t be delayed. Likewise, if Gum Pain is paired with loose teeth, persistent bleeding, or visible gum recession, those are common reasons people choose to book a professional evaluation.
At Stamboul Clinic, we see that clarity itself can be therapeutic: when patients understand the likely categories (irritation, inflammation, infection, dryness, or trauma), they feel less stuck in guesswork. Gum Pain often becomes less scary when it becomes more specific.
How Dentists Investigate Gum Pain: The Tools Behind the Answer
A thorough evaluation for Gum Pain typically starts with history: when it began, what triggers it, whether it’s localized or generalized, and what changed recently. That short timeline can be surprisingly diagnostic. For example, pain after a new filling may lead to a different line of thinking than pain that started during a stressful month with jaw clenching.
Clinicians also examine the gumline for inflammation, bleeding tendency, recession, and plaque accumulation. Periodontal probing can measure pocket depths around teeth. This helps identify whether the pain is linked to superficial irritation or deeper tissue involvement. When needed, dental radiographs can provide information about bone levels, hidden decay, or infection around tooth roots that might be contributing to Gum Pain.
In some cases, the source isn’t the gums at all. Referred pain from clenching, a cracked tooth, or sinus-related pressure can mimic gum discomfort. That’s one reason self-diagnosis is tricky: Gum Pain is a sensation with many possible origins, and the mouth is an expert at blending signals.
Turning Gum Pain Into Useful Information
Gum Pain is uncomfortable, but it’s also informative. It can arise from everyday irritation, plaque-driven inflammation, localized issues like food traps, or broader factors like dry mouth and hormonal shifts. The most helpful approach is usually a two-track mindset: aim for gentle comfort while also identifying patterns that point toward the root cause.
If there’s one takeaway, it’s that gums rarely complain without a reason. When Gum Pain persists, intensifies, or returns in cycles, getting a professional perspective can replace uncertainty with a plan. Stamboul Clinic’s philosophy is simple: listen carefully to the story your mouth is telling, then respond with evidence-based dentistry and clear communication.